Last Updated on: 19th September 2025, 12:43 pm
Melanoma In The Mouth
Melanoma in the mouth or oral Melanoma is a disease that, although rare, can have serious consequences if it is not detected in time. Patients often go to the dentist only when they experience symptoms and rarely undergo routine exams that could identify problems in the early stages. This article focuses on updating, improving, and adding more information to the topic of melanoma in the mouth, highlighting the importance of early detection while providing useful tips for oral self-examination.
What is Melanoma?
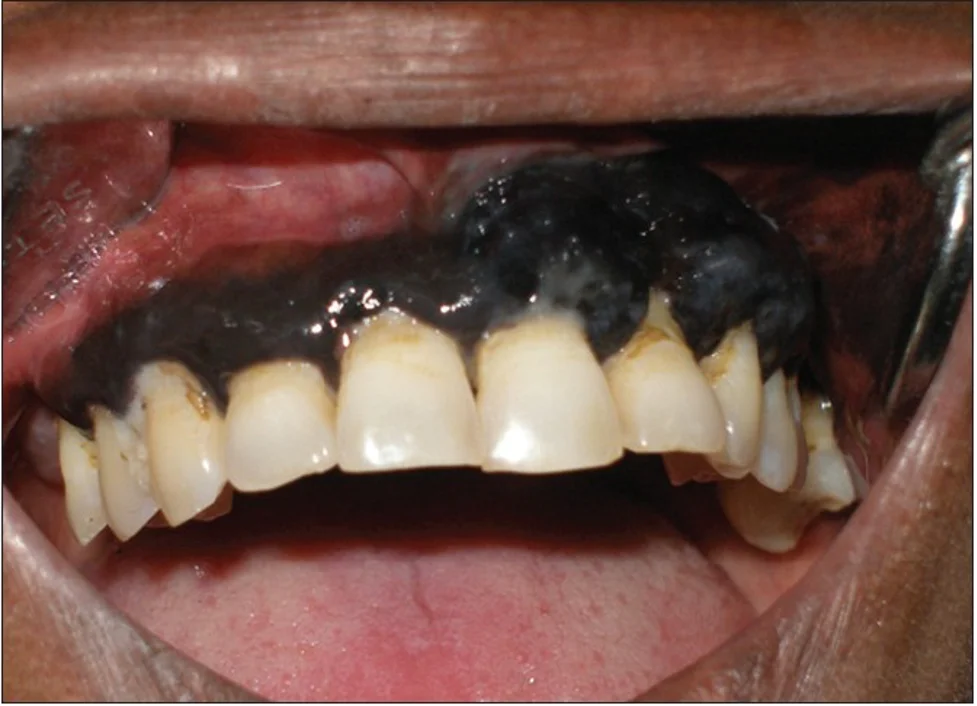
Melanoma is a pigmented lesion that can affect both the skin and the mucous membranes. It is generally associated with the skin, it can also manifest on the oral mucosa. It is considered the most serious type of skin cancer due to its potential to spread quickly if not treated in time. Excessive exposure to the sun’s UV rays is a major risk factor in the formation of skin melanoma, as it can alter pigment cells called melanocytes.
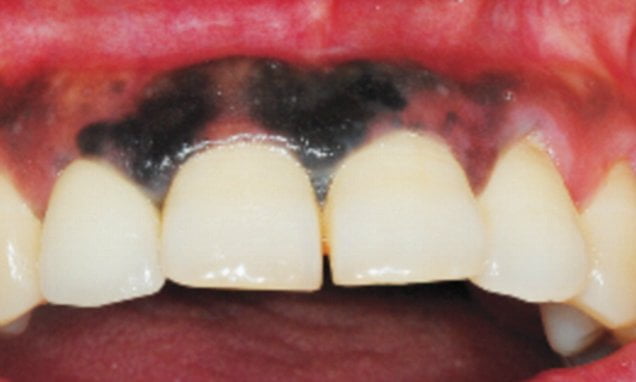
However, there are “hidden” melanomas that develop in areas of the body with little or no sun exposure, including the mucosa of the mouth. Detecting oral melanoma early is crucial for successful treatment. This type of melanoma often occurs on the palate and upper gums, but in its most aggressive form, it can be located on the jaw and tongue.
Patients sometimes remember having oral pigmentation for months or years before diagnosis, underscoring the importance of paying attention to early signs and not ignoring comments from doctors or dentists.
How it Presents
Melanoma in the mouth or oral melanoma is a rare disease, but it is essential to understand its extent and prevalence. Unlike its skin counterpart, it is not related to sun exposure since the oral mucosa is protected from ultraviolet light. According to updated data from the American Cancer Society, it is estimated that about 4,500 new cases of oral and pharyngeal cancer will be diagnosed in the United States in 2022. Of these cases, a significant proportion will be oral melanoma. Additionally, incidence rates vary by geographic region and sun exposure.
According to a report published in 2021, melanomas affecting the head and neck make up approximately 25% of all cases, although melanomas that develop on the mucosa are rare and represent less than 1% of the total cases.
Around 80% of oral malignant melanomas originate in the mucosa of the upper jaw and are most frequently found on the palate. However, they can also appear on the lips, gums, or tongue.
Causes
The exact causes of melanoma in the mouth remains unclear and do not appear to be directly related to sun exposure. Possible causes have been proposed such as irritation caused by dentures, alcohol consumption, smoking, and genetic mutations. However, experts have not yet established a direct relationship between any of these factors and the development of melanoma in the mouth.
Symptoms Of Having Melanoma In The Mouth
The first signs of melanoma in the mouth usually include swelling accompanied by a brown or black spot or a nodular lesion, which may present gray, red, or purple areas or loss of pigmentation, that is, a lack of color.
● A spot refers to an area of skin that is flat and without abnormal coloration, maintaining its normal texture and thickness.
● The primary tumor may be surrounded by groups of additional tumor cells, known as satellite tumors.
● Similar to cutaneous melanomas, oral melanoma may show irregular borders and an asymmetric shape.
It is important to note that, in general, oral melanomas tend to manifest few symptoms in the early stages, and around 33% of people have no symptoms at the time of diagnosis. Symptoms that may arise in later stages include redness of the mucosa, known as erythema, and ulceration.
Diagnosis and Treatment For Melanoma In The Mouth
Diagnosing oral melanoma involves a series of steps and tests performed by healthcare professionals, particularly dentists, and specialists who can perform oral cancer surgery. Here is how the diagnosis of oral melanoma is made:
1. Visual Evaluation with the “ABCD” system: Doctors use the “ABCD” system to identify characteristics of melanoma:
A: Asymmetry.
B: Irregular edge with notches or indentations.
C: Color variations, such as red, white, and blue.
D: Diameter greater than 0.6 millimeters.
2. Biopsy: A tissue biopsy is performed for a definitive diagnosis. This sample is examined in the laboratory.
3. Imaging studies: In some cases, imaging studies such as computed tomography (CT) or magnetic resonance imaging (MRI) may be ordered to evaluate the extent of the tumor and check if it has spread.
4. Lymph node evaluation: If the diagnosis of oral melanoma is confirmed, an evaluation of nearby lymph nodes may be performed to determine if the cancer has spread to these areas.
5. Staging: Once all the information has been gathered, the stage of your oral melanoma will be determined to help doctors plan the right treatment.
Treatment for oral melanoma largely depends upon the stage at which it is diagnosed. In the early stages, surgery to remove melanoma is the main option. In more advanced cases, additional therapies, such as radiation therapy, immunotherapy, and targeted therapies, may be necessary to prevent the cancer from spreading. Importantly, early detection significantly increases the chances of successful treatment.
How can we Detect It in Time?
Early detection for Melanoma in the mouth is essential for a favorable prognosis. While regular visits to the dentist are the best way to identify problems in the early stages, there are steps you can take at home to self-examine:
● Use a mirror and good lighting to examine all available oral mucosal surfaces.
● Use a 2×2 gauze pad and retract your tongue while moving it from side to side to get a clear, unobstructed view.
● If you notice any unusual spots or lesions, even if they are small, make an appointment with your dentist or doctor immediately for diagnostic tests.
Additionally, the Oral Cancer Foundation recommends visiting your dentist at least twice a year for professional evaluations, which increases the chances of detecting any abnormalities early on. Don’t underestimate the importance of these regular checkups, as they can make a difference in your oral and overall health.
Conclusion
Oral melanoma is a serious disease that can seriously affect a person’s oral and general health. Although it is less common than cutaneous melanoma, its early detection is essential for a favorable prognosis. Risk factors, such as sun exposure, family history, and certain habits, play a role in its development, but the exact causes are not yet fully understood.
Early diagnosis and proper medical care are essential to effectively address oral melanoma. Dental health professionals play a crucial role in initial detection, and regular exams are essential. Prevention, regular dental care, and seeking medical attention for any changes in the mouth are vital to reducing risks and addressing the disease effectively.
Frequently Asked Questions
What are the most common symptoms of oral melanoma and when should I worry about them?
Initial symptoms of oral melanoma may include swelling along with a brown or black nodular lesion with gray, red, purple areas, or depigmentation. You should be concerned about these symptoms if they persist or change over time, as early detection is essential.
What is the importance of regular dental exams in the early detection of oral melanoma?
Regular dental exams play a crucial role in the early detection of oral melanoma, as dental health professionals can identify suspicious lesions during these checkups. This allows for early diagnosis and more effective treatment.
What are the main risk factors that increase the likelihood of developing oral melanoma?
Risk factors include prolonged unprotected sun exposure, family history of skin cancer, smoking, and excessive alcohol consumption. These factors may increase susceptibility to oral melanoma.
What treatment options are available for oral melanoma and what is the typical prognosis for sufferers?
Treatment options vary, depending upon the stage of oral melanoma and include surgery, radiation therapy, immunotherapy, and targeted therapies. The prognosis depends on the stage at which it is diagnosed;, but early detection is usually associated with better outcomes. Specialized medical care is essential for a favorable prognosis.
Share:
References
1. Ulloa, P., Fredes, F., & Resumen, C. (2016). Manejo actual de la xerostomía. Revista Otorrinolaringología y Cirugía de Cabeza y Cuello, 76(2), 243–248. http://www.scielo.cl/scielo.php?script=sci_arttext&pid=S0718-48162016000200017&lng=es&nrm=iso&tlng=es
2. Gutiérrez, L., & Herrera, D. B. S. (2018). Hiposalivación asociada al consumo de medicamentos. [Tesis de grado]. Universidad Santo Tomás. https://repository.usta.edu.co/bitstream/handle/11634/16154/2018lauragutierrezsharonbarreradarlyherrera.pdf?sequence=1&isAllowed=y
3. Galindo, P., Yohana, M., Javier, E., & Nieto, L. (s.f.). Phenomenological approach to the side effects of medicines in swallowing in the elderly population. www.revistaavft.com
4. Biblioteca Nacional de Medicina de los EE. UU. (2020). Hipertensión arterial – adultos: MedlinePlus enciclopedia médica. https://medlineplus.gov/spanish/ency/article/000468.htm
5. Department of Scientific Information, Evidence Synthesis & Translation Research, ADA Science & Research Institute L. (2020). Hypertension. https://www.ada.org/en/member-center/oral-health-topics/hypertension
6. Mayo Clinic. (2021). Diuréticos. https://www.mayoclinic.org/es-es/diseases-conditions/high-blood-pressure/in-depth/diuretics/art-20048129
7. Bethesda (MD): Biblioteca Nacional de Medicina (EE. UU.). (2018). Espironolactona: MedlinePlus medicinas. https://medlineplus.gov/spanish/druginfo/meds/a682627-es.html
-
Nayibe Cubillos M. [Author]
Pharmaceutical Chemestry |Pharmaceutical Process Management | Pharmaceutical Care | Pharmaceutical Services Audit | Pharmaceutical Services Process Consulting | Content Project Manager | SEO Knowledge | Content Writer | Leadership | Scrum Master
View all posts
A healthcare writer with a solid background in pharmaceutical chemistry and a thorough understanding of Colombian regulatory processes and comprehensive sector management, she has significant experience coordinating and leading multidisciplina...Recent Posts