Last Updated on: 27th December 2025, 04:59 am
Every year, 380,000 new cases of oral cancer are diagnosed across the world, potentially requiring people to undergo oral cancer surgery. This was stated by the World Health Organization in November of 2022.
Regarding the prevalence of this disease in the United States, the National Institute of Dental and Craniofacial Research reported that in that country, more than 53,000 cases are diagnosed annually and oral cancer registers a higher prevalence in people over 40 years of age.
Oral cancer is a consequence of the DNA mutation of the cells in the oral cavity, a change that causes adverse health effects due to abnormal behaviors manifested by the cells involved and their corresponding lesions or ulcers in different parts of the mouth. It could be the lips, gums, tongue, inner cheeks, palate (roof of the mouth), or floor of the mouth (under the tongue).
Oral cancer may be brought on by soft palates. To find out more, you can read the article.
The agglomeration of cancer cells can eventually form a tumor and cause the disease to spread to other areas of the neck, head, or body. This expansive process is known as metastasis.
What is Oral Cancer Surgery?
If oral cancer is diagnosed on time, it is possible to apply different treatment alternatives and one is surgery, depending upon the progress and state of the disease.
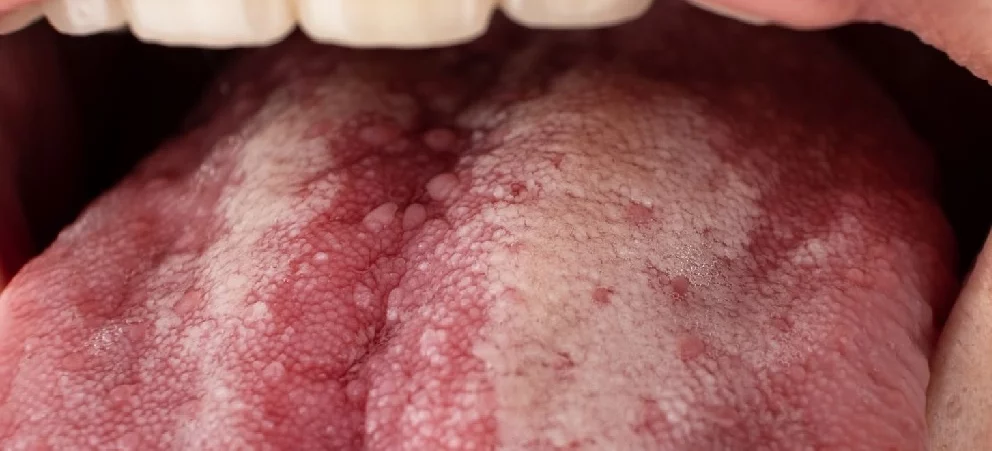
Surgery to treat oral cancer removes any tissue that may be affected. Sometimes nearby lymph nodes will also need to be removed to prevent the spread of the disease.
Surgery for the treatment of oral cancer can be complemented with radiotherapy or chemotherapy sessions, with the purpose of eliminating the remaining cancer cells and reducing the risk of recurrence.
How is Oral Cancer Diagnosed?
To make the diagnosis of oral cancer you have two options:
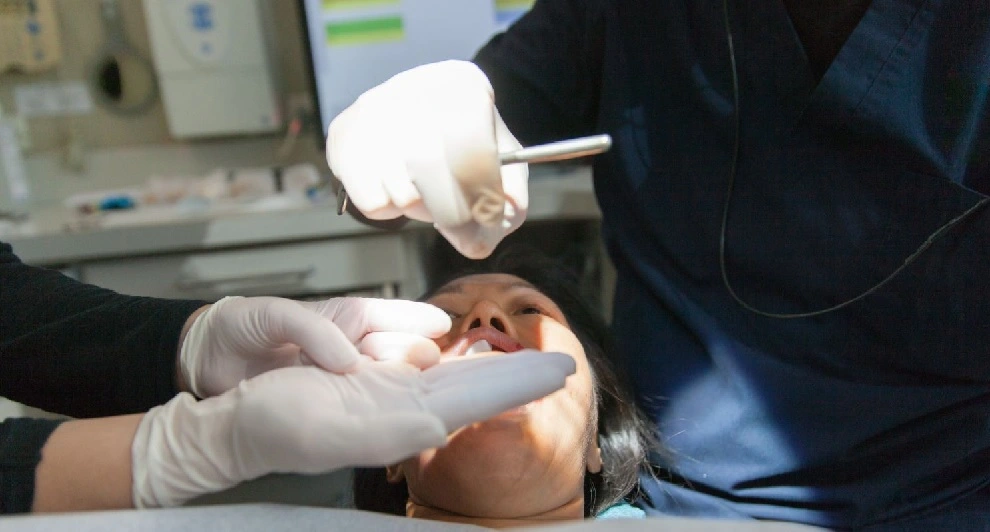
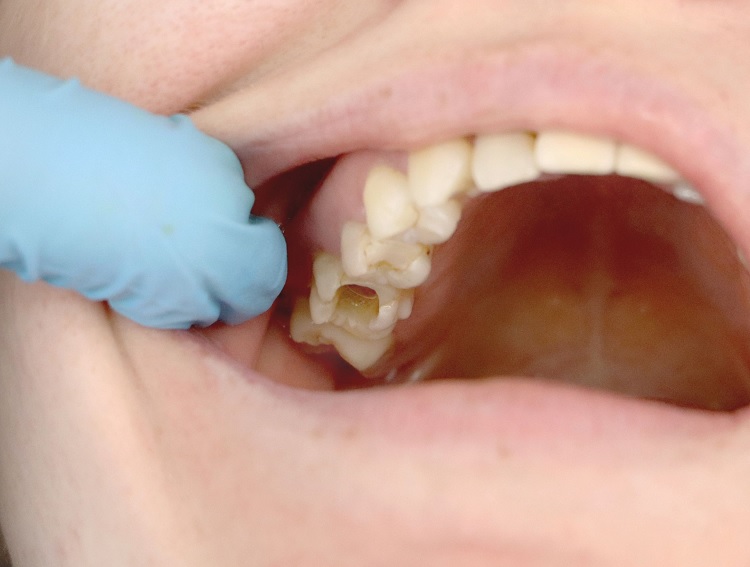
• A physical examination of the lips and mouth by the dentist or doctor to look for irritation, sores, or white patches.
• The removal of a piece of tissue for biopsy. This test is performed if any suspicious tissue is found. The tissue sample is analyzed in the laboratory to see if there are any signs of cancer.
After the diagnosis, the health professional will perform the necessary tests to determine the stage of the cancer.
One of the procedures to establish the stage of development is endoscopy, which is done with the help of a micro-camera to observe the throat and check for signs of metastasis in that area of the body.
Another option is diagnostic imaging, which may include an X-ray, tomography, magnetic resonance imaging, and positron emission tomography (PET Scan), among others.
What are the Types of Surgery for Oral Cancer?
There are different types of interventions; each addresses the diagnosis, depending upon the size, location of the cancer, and its stage of evolution.
1. Laser ablation
Uses a high-energy laser to burn and vaporize the affected tissue. It is a precise and less invasive method than conventional surgery, and it can be useful to treat small tumors.
2. Removal
The tumor and a part of the nearby tissue are removed to ensure a greater probability of success of the intervention. If the tumor is large, it may be necessary to remove a part of the affected jaw bone (mandibular resection).
3. Neck dissection
If the risk that cancer cells have spread to the lymph nodes in the neck is identified – or there is a risk of this happening – the lymph nodes and nearby tissue are removed to prevent the spread of the disease. Additional treatment may be required after surgery.
4. Micrographic surgery
Also called Mohs surgery, it consists of removing the affected tissue in very thin layers. Each layer is analyzed to identify if there are cancer cells. The necessary layers of tissue are removed until clean areas not affected by the disease are reached. This method reduces the amount of tissue that is removed, but it takes more time.
5. Reconstructive surgery
After resection or removal surgery, this intervention may be necessary to restore the shape and function of the mouth. In this case, skin or bone grafts are used, or the placement of dental or mandibular prostheses.
6. Glossectomy
It is the removal of the tongue and may be necessary to treat cancer in this sensory organ that is part of the oral cavity. In the case of small tumors, a partial glossectomy is performed. Larger tumors may require a total glossectomy.
Preparing for Oral Cancer Surgery
It is essential to speak with the doctor to identify other therapeutic alternatives or to define the timeframe of the intervention. This dialogue should cover all the concerns you have: risks during the intervention, additional subsequent treatments, consequences if the surgery is not assumed, probability of success, recovery time, etc.
The waiting time between diagnosis and surgical intervention depends upon the progress of the disease, that is, the stage in which it is found. In some cases, it is vital to operate as soon as possible. Other diagnoses may call for radiotherapy or chemotherapy before surgery.
In the preoperative phase, the medical team provides detailed information about the procedure. Then the patient authorizes the surgery, considering the risks, side effects, and benefits, among other aspects. This is known as informed consent and the corresponding document must be signed.
It is also required to order some clinical tests to determine if the person is in suitable health condition for surgery.
The doctor will provide corresponding instructions for fasting before the intervention, thus avoiding inconveniences with anesthesia. This can be of local, regional, or general administration, depending upon the magnitude of the surgery.
Recovering from Oral Cancer Surgery
It is likely that when you wake up from surgery, you will not want to eat or drink. With the passage of postoperative time, the digestive system will recover its normal activity. In the first few days, a bland, liquid-based diet is usually administered and will evolve as the recovery process progresses.
Pain, inflammation, difficulty in eating and speaking, and changes in the appearance of the mouth and face are some of the side effects of surgical intervention. Generally, these are temporary and are treated with medication.

The intervention has risks of bleeding and infection. In addition, it affects the physical appearance and the ability to speak. These circumstances are treated with complementary therapies.
After the intervention, care is required to ensure a successful recovery and prevent complications. For this purpose, the surgeon will give instructions on the care of the operated area, which must be followed.
The diet during recovery, as well as the advised oral hygiene practice, are part of the instructions for the recovery period.
When is it Appropriate to Consult with the Doctor?
Oral cancer presents signs and symptoms that can be detected quickly:
• Mouth pain
• Earache
• Difficulty or pain when swallowing
• A sore on the lips or mouth that does not heal
• A white or reddish patch on the inside of the mouth
• A growth or lump inside the mouth

If any of these signs are perceived, the doctor or dentist should be consulted so that the required assessment and tests can be carried out to determine the diagnosis.
Acting on Time is Giving an Option for Oral Health
At the first sign of alarm, consult your healthcare professional. This will afford a greater opportunity for an early diagnosis and to take the indicated treatment route in a proactive and non-reactive way. In this way, more complex situations for oral health and comprehensive well-being are avoided.
Frequently Asked Questions
What is the survival rate for oral cancer after surgery?
For Stage I oral cancer, the 5-year survival rate is around 83%. For Stage II, the survival rate drops to about 66%, and for Stage III, it further decreases to roughly 45% over five years. It’s crucial to remember that these statistics are general estimates and do not consider individual factors like age, overall health, and specific treatment methods.
What type of surgery is performed for mouth cancer?
The procedure is known as a maxillectomy. Depending on the extent of the cancer, the surgery may involve removing all of the bones in the roof of the mouth (total maxillectomy) or only a portion of the bones in the roof of the mouth (partial maxillectomy).
Is speaking possible after mouth cancer surgery?
Your voice might become huskier, quieter, or sound as if you have a constant cold. Some individuals may lose their voice altogether. Pronouncing certain words may become challenging, or you might slur some words. These issues can be temporary and may improve once the post-surgery swelling subsides.
Can you fully recover from oral cancer?
And that’s a very difficult question because there is no absolute time point where we can say that you are cured of your cancer. But for oral cancer, most of the cancers will come back within the first two years of treatment.
Is surgery for oral cancer painful?
After surgery for oral cancer, it is common to experience pain. During the initial weeks post-surgery, you will likely feel significant discomfort. However, this pain can be effectively managed with medication.
Share:
References
1. American Cancer Society (March 9, 2018) Surgery for Oral Cavity and Oropharyngeal Cancer / https://www.cancer.org/es/cancer/tipos/cancer-de-orofaringe-y-de-cavidad-oral/tratamiento/cirugia.html
2. American Cancer Society (October 2, 2019) Preparing for and recovering from cancer surgery / https://www.cancer.org/es/cancer/como-sobrellevar-el-cancer/tipos-de-tratamiento/cirugia/recuperacion-despues-de-la-cirugia-contra-el-cancer.html
3. Johnson Shannon (September 1 of 2020) Oral Cancers / https://www.healthline.com/health/oral-cancer
4. Mayo Clinic (October 2022) Mouth cancer – Overview / https://www.mayoclinic.org/diseases-conditions/mouth-cancer/symptoms-causes/syc-20350997#:~:text=Surgery%20is%20the%20main%20treatment,alone%20may%20be%20enough%20treatment
5. Mayo Clinic (April 15, 2022) Mouth cancer – Diagnosis / https://www.mayoclinic.org/diseases-conditions/mouth-cancer/diagnosis-treatment/drc-20351002
6. National Institute of Dental and Craniofacial Research (s.f.) Oral Cancer / https://www.nidcr.nih.gov/health-info/oral-cancer
7. WHO (November 18, 2022) The WHO highlights that neglect of oral health affects almost half of the world’s population / https://www.who.int/es/news/item/18-11-2022-who-highlights-oral-health-neglect-affecting-nearly-half-of-the-world-s-population#:~:text=Se%20calcula%20que%20la%20periodontitis,nuevos%20casos%20de%20c%C3%A1ncer%20bucal
-
Nayibe Cubillos M. [Author]
Pharmaceutical Chemestry |Pharmaceutical Process Management | Pharmaceutical Care | Pharmaceutical Services Audit | Pharmaceutical Services Process Consulting | Content Project Manager | SEO Knowledge | Content Writer | Leadership | Scrum Master
View all posts
A healthcare writer with a solid background in pharmaceutical chemistry and a thorough understanding of Colombian regulatory processes and comprehensive sector management, she has significant experience coordinating and leading multidisciplina...Recent Posts