Last Updated on: 27th December 2025, 06:00 am
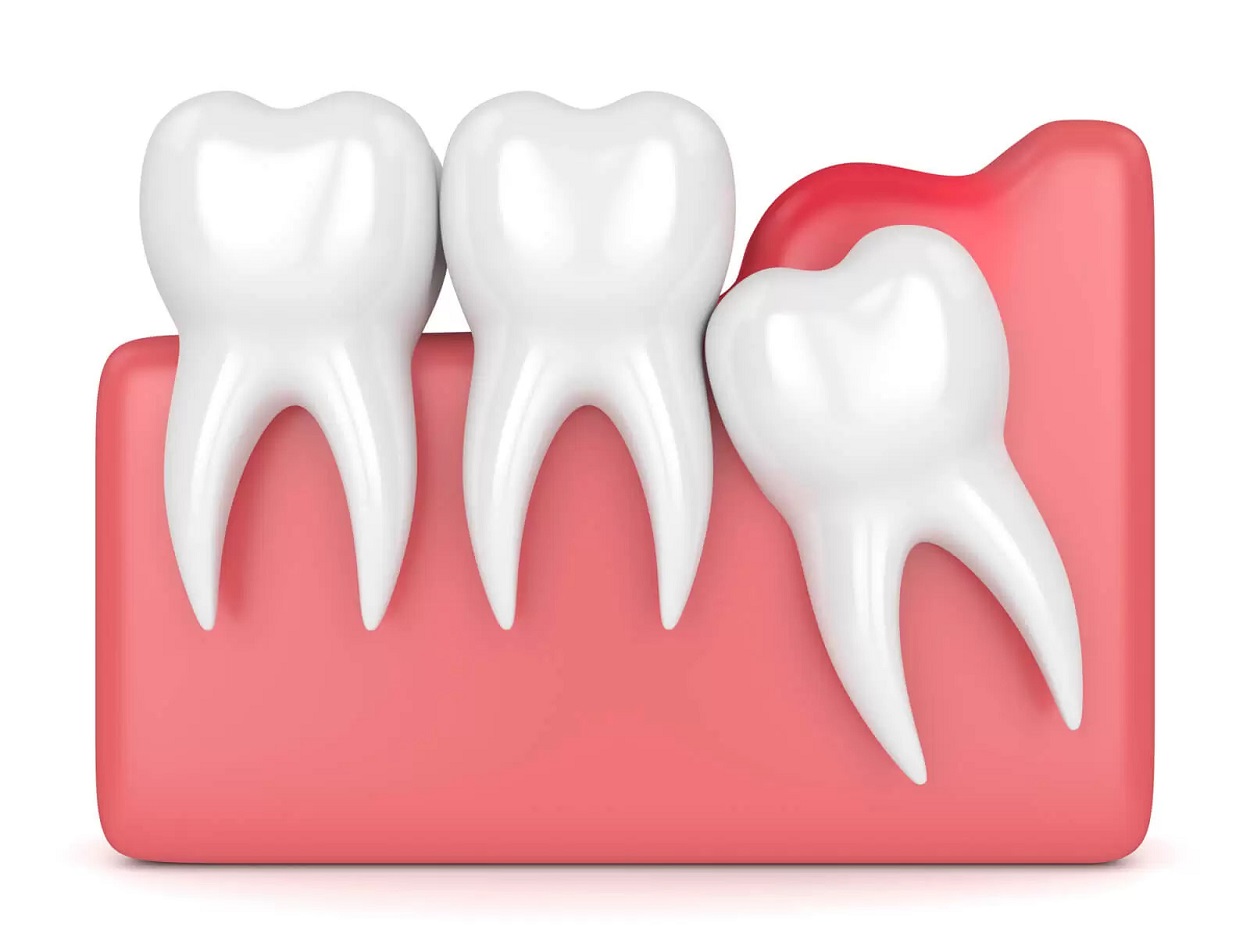
Pericoronitis occurs around the gums of emerging teeth. It happens often with the lower third molars, also called wisdom teeth. The most affected patients are young people between the ages of 15 and 25 since at this age, these molars appear.
What is Pericoronitis?
The term pericoronitis is used for an inflammation of the gums around an erupting tooth. It does not commonly happen in all teeth; rather, it tends to occur frequently in those that come in slowly or do not have enough space to emerge, as often happens with wisdom teeth.
What Causes Pericoronitis?
Sometimes, when the wisdom teeth are coming in, a space or pocket can form between the gum and the tooth.t is easy for food to accumulate, causing an infection. It is also common that when the gum next to the tooth coming out is inflamed, it increases in size and is injured when biting by the opposite teeth. This further increases the inflammation and discomfort it produces.
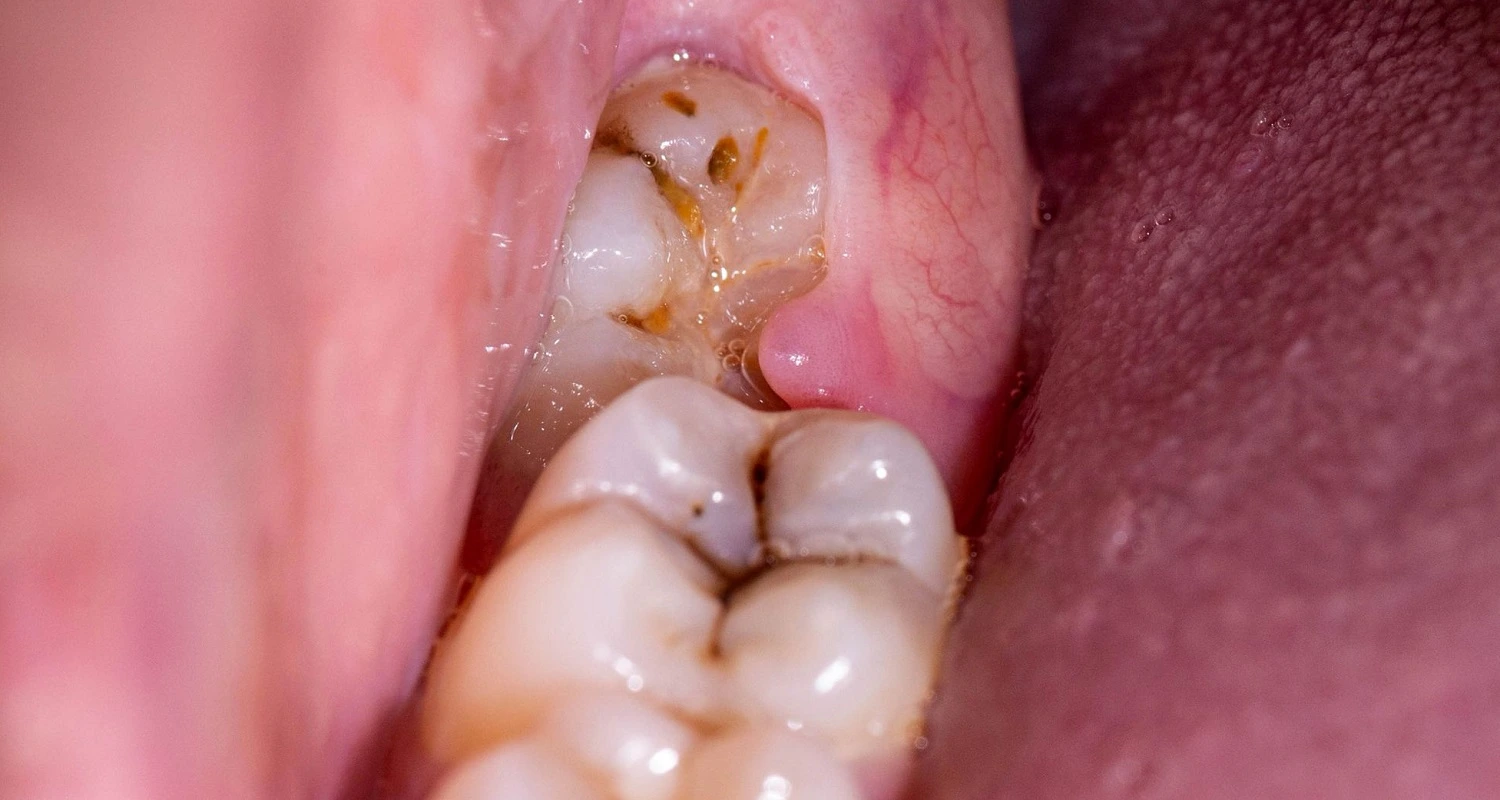
Signs and Symptoms of Pericoronitis
People affected by pericoronitis may present:
• Pain in the area where the tooth is coming out
• Inflammation inside and outside the mouth
• Bad mouth taste
• Bad breath
• Pain and swelling in the neck lymph nodes (small nodules that become inflamed when there are infections)
• Difficulty opening the mouth
• Pain when biting
• Sore throat
• General malaise
• Fever
How to Prevent Pericoronitis?
Since the inflammation is largely caused by food accumulating in the area, the secret is to keep that little pocket free of food debris until the tooth is fully out or can be extracted. It is advisable to perform adequate hygiene in the area. In addition to tooth brushing, it is advisable to undertake pressure washings with a syringe and saline solution, to ensure that food remains are removed.

Treatment of Pericoronitis
If the molar does not have enough space, the appropriate treatment would be to extract it. However, as long as there is pain and inflammation, it is not appropriate to perform this procedure, for two reasons:
1. Increased risk of infection: Manipulating and anesthetizing an area with an acute infection can cause it to spread to other parts of the body, making it even worse, more serious, and difficult to treat.
2. Anesthesia does not work properly: In infected and highly inflamed tissues, anesthesia does not work properly, so it could be a very painful and difficult procedure.
Therefore, first, pericoronitis should be treated, and when the infection and inflammation are controlled, the tooth can be removed. The treatment of pericoronitis depends upon how advanced the infection is:
1. Washing the area: In its initial phases when there is pain and mild inflammation, it is possible to deflate the gum’ the pain decreases only by a correct washing of the gums in the area where food residue accumulated. The dentist will use a chlorhexidine-based solution to disinfect the space formed between the gum and the tooth.
2. Anti-inflammatories and analgesics: If the pain is very strong, the dentist may prescribe medications either taken by mouth or injected to reduce the inflammation and pain.
3. Operculectomy: A procedure that consists of removing the gum partially covering the tooth to properly clean the affected area and prevent food debris and bacteria from accumulating. The treating dentist could choose to perform this procedure if it is not feasible to remove the tooth just yet.
4. Antibiotic therapy: If the infection is very advanced, it may be necessary to administer antibiotics. However, they must be prescribed by a dentist as depending upon the progress of the infection and other medications the patient is taking, a different antibiotic will be indicated. For very advanced infections, the treating professional could choose to use intravenous antibiotics.
What Happens if Pericoronitis is not Treated on Time?
If the infection progresses until pus has accumulated in the area, it could migrate to the neck area, just under the jaw, and then generate very severe inflammation that prevents proper breathing. This condition is known as Ludwig’s angina, and it could be life-threatening. It is vital that pericoronitis be controlled in its early stages and you go to the dentist if there are warning signs.
Pericoronitis can potentially lead to gum disease if not managed properly or if it becomes a chronic issue. Pericoronitis is a condition in which the gum tissue around a partially erupted tooth, often a wisdom tooth, becomes inflamed and infected. This condition can cause symptoms such as pain, swelling, redness, and difficulty in opening the mouth.
To learn about gum disease treatment, you can check out this article.
When to See the Dentist?
The treatment of pericoronitis and any infection should always include eliminating the cause of the infection, in addition to any antibiotics and anti-inflammatories prescribed for oral administration. washing the area, the patient continues to experience severe pain, swelling of the face, difficulty eating, fever, or general malaise, they should see a dentist as soon as possible to undertake the appropriate treatment.
Conclusion
Pericoronitis frequently occurs when the third molars begin erupting, especially the lower ones. As it is caused by the accumulation of food between the tooth and the gums that partially cover it while it is erupting, the best way to prevent and treat it in its initial phases is to remove the food residue and disinfect the area. However, when the condition is not treated in time, it can become a dangerous infection that could even compromise life. Therefore, it is important to see a dentist when detecting the alarm signs mentioned above, especially fever and malaise.
Frequently Asked Questions
What is the primary cause of pericoronitis?
Pericarditis is often caused by an infection such as:
● Viral infections that cause chest colds or pneumonia.
● Bacterial infections (less common).
● Some fungal infections (rare).
What causes pericoronitis?
Pericoronitis is an intraoral inflammatory process resulting from an infection of the gingival tissue surrounding or covering an erupting or partially erupted tooth. It is most commonly associated with the eruption of mandibular third molars, although it can occur with any erupting teeth.
Can pericoronitis resolve on its own?
Unfortunately, pericoronitis does not go away on its own. If left untreated, it can become dangerous in just a couple of weeks. Usually, either the tissue flap or the wisdom tooth needs to be removed. If an infection is present, an antibiotic will also be necessary.
What happens if pericoronitis is left untreated?
It’s important to note that pericoronitis shouldn’t be left untreated for too long. It can lead to various health complications, including life-threatening conditions such as Ludwig’s angina, which blocks the airway, and sepsis, which spreads the infection into the bloodstream.
Share:
References
1. Schalch, TO (Sep 8, 2020.). Interventions for Early-Stage Pericoronitis: Systematic Review of Randomized Clinical Trials. MDPI. https://www.mdpi.com/2079-6382/11/1/71
2. Kwon G, Serra M.(Nov 21, 2022). Pericoronitis. National Library of Medicine. https://www.ncbi.nlm.nih.gov/books/NBK576411/
3. Pericoronitis: Symptoms, Causes & Treatment. (Nov 9, 2022). Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/24142-pericoronitis
4. Schalch, TO (Jan 8, 2022). Interventions for Early-Stage Pericoronitis: Systematic Review of Randomized Clinical Trials. MDPI. https://www.mdpi.com/2079-6382/11/1/71
5. Al Farabi Clinics, J., & Arabia, S. (Nov 17, 2022). Etiology, Evaluation, and Treatment of Pericoronitis. https://www.johs.com.sa/admin/public/uploads/187/114_pdf.pdf
6. Huang, X., Zheng, H., An, J., Chen, S., Xiao, E., & Zhang , Y. (Aug 5, 2020). Microbial Profile During Pericoronitis and Microbiota Shift After Treatment. Frontiers in microbiology, 11, 1888. https://doi.org/10.3389/fmicb.2020.01888
7. Schmidt, J., Kunderova, M., Pilbauerova, N., & Kapitan, M. (Jun 24, 2021). A Review of Evidence-Based Recommendations for Pericoronitis Management and a Systematic Review of Antibiotic Prescribing for Pericoronitis among Dentists: Inappropriate Pericoronitis Treatment Is a Critical Factor of Antibiotic Overuse in Dentistry. International journal of environmental research and public health, 18(13), 6796. https://doi.org/10.3390/ijerph18136796
-
Nayibe Cubillos M. [Author]
Pharmaceutical Chemestry |Pharmaceutical Process Management | Pharmaceutical Care | Pharmaceutical Services Audit | Pharmaceutical Services Process Consulting | Content Project Manager | SEO Knowledge | Content Writer | Leadership | Scrum Master
View all posts
A healthcare writer with a solid background in pharmaceutical chemistry and a thorough understanding of Colombian regulatory processes and comprehensive sector management, she has significant experience coordinating and leading multidisciplina...Recent Posts