Last Updated on: 3rd April 2026, 11:32 am
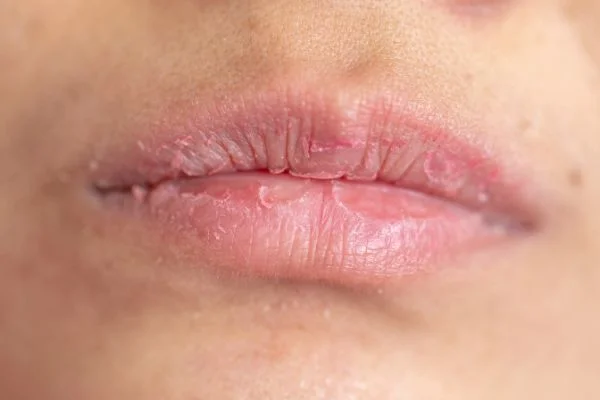
Trench mouth is a severe gum infection caused by harmful bacteria, often linked to poor oral hygiene, stress, and weakened immunity. It develops quickly, causing intense pain, bleeding, ulcers, and bad breath. Without timely treatment, it can lead to permanent gum damage, tooth loss, and serious systemic complications.
Frequently, we hear about cavities and toothaches, but there are many other mouth diseases associated with soft tissues, such as gingivitis.
Gingivitis is a gum infection caused by a buildup of plaque and tartar, leading to an imbalance of bacteria that live in the oral cavity and causing problems such as bad breath, red, sore, bleeding, and swollen gums, and can develop into a trench mouth.
What is a trench mouth?
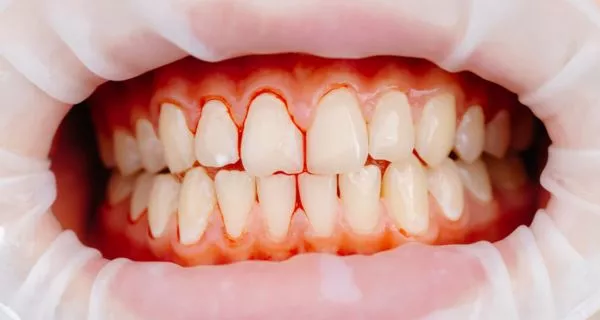
Also known as acute necrotizing ulcerative gingivitis (ANUG) or Vincent’s stomatitis, trench mouth is a bacterial infection of the gums, a more severe and advanced form of gingivitis; it can appear quickly and cause serious damage to the teeth and gums, and even spread to other areas of the mouth such as cheeks, lips or jaw.
The name of this disease comes from World War I, when soldiers were exposed to precarious conditions, without access to medical or dental care, living in trenches dug into the ground and without the elements to perform proper oral hygiene, the reason why many of those soldiers presented serious gum diseases.
Why does a trench mouth appear?

This disease occurs when the balance of bacteria in the mouth is disrupted, and there is an excess of pathogenic bacteria.
Who is most affected by trench mouth?
Trench mouth affects between 0.5% and 11% of the population. It is more commonly found in:
- Young adults between the ages of 15 and 35
- People with autoimmune diseases such as HIV.
Additionally, this disease is common in places where people have little or no access to dental health services, and where there is a high incidence of malnutrition.
What are the main risk factors?
The main cause of this condition is poor oral hygiene, but there are other risk factors associated with the appearance of trench mouth:
- High levels of stress
- Malnutrition, vitamin and mineral deficiencies
- Smoking and alcohol abuse
- Weak immune system (cancer or other diseases requiring immunosuppressants)
- Infections in the throat, teeth or mouth
- Having diseases such as diabetes or autoimmune diseases like HIV.
- Having gum injuries
- Having previously had gingivitis.
What are the signs and symptoms of trench mouth?

Symptoms of trench mouth usually appear suddenly and rapidly. There is often severe and intense pain that affects one or several areas of the gum. Other common symptoms include:
- Bad breath, noticeable due to its unpleasant odor
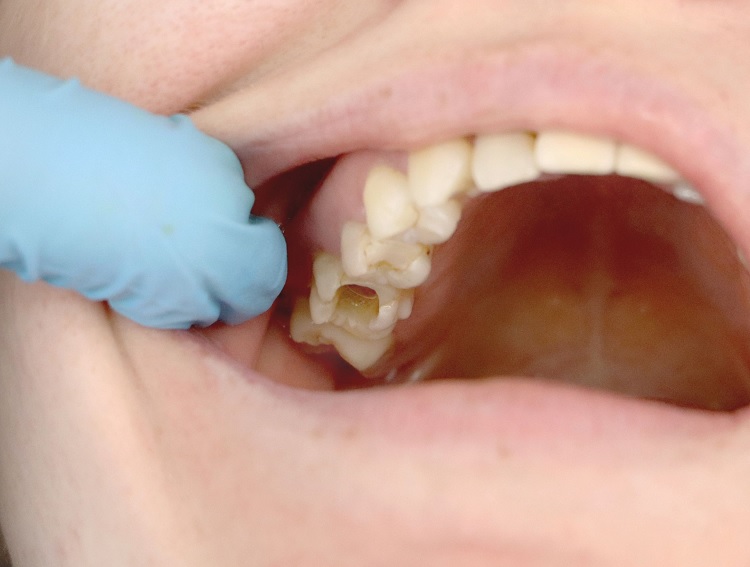
- Ulcers: crater-like sores between the teeth and gums, filled with plaque and food debris
- Severe pain
- Red and inflamed gums
- Bleeding gums even with the slightest touch
- Unpleasant taste in the mouth that is perceived by the patient. Some describe it as a metallic taste like iron.
- Destruction of the gum tissue around the teeth
- Membrane of white, yellow, or gray color that covers the ulcerated papillae, which appear reddish and bleeding
- Swollen lymph nodes around the head, neck, or jaw
- Fatigue
- Severe bleeding of the gums in response to any pressure or irritation, including brushing.
- Fever
What happens if trench mouth is not treated?

If left untreated, this disease can lead to one or several of the following complications:
- Damage to the soft tissue at the gum level and spread to other areas of the mouth such as the jaw, cheeks, and lips.
- Irreversible damage to the gums and bone that can lead to loosening and loss of teeth.
- The patient may experience difficulty in performing daily activities such as talking, eating, and swallowing, leading to weight loss and dehydration.
- Bacteria can infiltrate the bloodstream (bacteremia) and spread to the rest of the body, potentially causing death.
- In very severe cases, oral gangrene may develop.
When should you see a dental professional?
It is recommended to visit the dentist at least twice a year (every 6 months). This habit will help you maintain good oral health, as well as diagnose and treat any diseases that may arise in a timely manner.
If you have not developed this habit and have one or several of the symptoms described in this article, you should see a dentist as soon as possible. The healthcare professional will perform a clinical examination, and in some cases, may require x-rays to determine the degree of infection progression.
How is trench mouth treated?
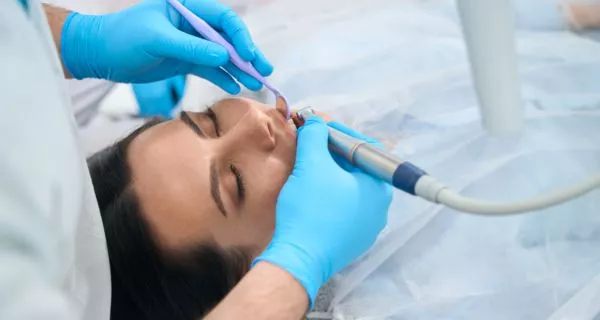
Early treatment helps eliminate infection and relieve symptoms, preventing long-term damage.
Treatment may include:
- Antibiotics
- Pain relievers
- Professional dental cleaning
- Surgical treatment in advanced cases to restore gum health
Treating trench mouth promptly significantly reduces the risk of complications and future oral diseases.
You can find more information about diagnosis, treatment, and prevention in our article “Treatment of Trench Mouth”, available on our website. Thank you for reading.
Frequently Asked Questions
What is a trench mouth?
What's the difference between a thrush and trench mouth?
Can you get a trench mouth from kissing?
Can children develop trench mouth?
Can trench mouth be completely cured?
Voice and Search (Q&A)
Is trench mouth dangerous?
Yes, untreated trench mouth can cause permanent gum damage, tooth loss, bone destruction, and serious systemic infections if ignored.
Is trench mouth the same as gingivitis?
No, trench mouth is a more severe, rapidly progressing infection that can develop from untreated gingivitis.
Can trench mouth be prevented?
Yes, it can be prevented with good oral hygiene, regular dental visits, healthy nutrition, stress management, and avoiding smoking.
Share
References
1. Burch, K. (2025, October 20). Symptoms of gum sores. Verywell Health. https://www.verywellhealth.com/gum-sores-symptoms-and-complication-6374334
2. Chaubal, T., & Bapat, R. (2017). Trench Mouth. The American Journal of Medicine, 130(11), e493-e494. https://doi.org/10.1016/j.amjmed.2017.05.020
3. Krans, B. (2018, September 29). Trench Mouth. Healthline. https://www.healthline.com/health/trench-mouth
4. Malek, R., Gharibi, A., Khlil, N., & Kissa, J. (2017). Necrotizing ulcerative gingivitis. Contemporary Clinical Dentistry, 8(3), 496. https://doi.org/10.4103/ccd.ccd_1181_16
5. Ubertalli, J. T. (2022). Acute Necrotizing Ulcerative Gingivitis (ANUG). MSD Manual Professional Edition. https://www.msdmanuals.com/professional/dental-disorders/periodontal-disorders/acute-necrotizing-ulcerative-gingivitis-anug
-
Nayibe Cubillos M. [Author]
Pharmaceutical Chemestry |Pharmaceutical Process Management | Pharmaceutical Care | Pharmaceutical Services Audit | Pharmaceutical Services Process Consulting | Content Project Manager | SEO Knowledge | Content Writer | Leadership | Scrum Master
View all posts
A healthcare writer with a solid background in pharmaceutical chemistry and a thorough understanding of Colombian regulatory processes and comprehensive sector management, she has significant experience coordinating and leading multidisciplina...Recent Posts