Last Updated on: 4th May 2026, 11:48 am
Amoxicillin is considered the first-line antibiotics for tooth infections in patients without penicillin allergies. For those who are allergic, clindamycin is often the preferred alternative. However, antibiotics do not replace necessary dental procedures like drainage or extractions, and they should only be used when prescribed by a professional.
That throbbing pain in your jaw that keeps you up at night, the swelling that won’t go away, the feeling that something is very wrong, a tooth infection is one of the most uncomfortable dental emergencies a person can experience. And one of the first questions people ask is: “Do I need an antibiotic?”
The answer isn’t always straightforward. Not every tooth infection requires antibiotics, and choosing the wrong treatment can actually slow your recovery. In this guide, you’ll learn exactly when antibiotics are needed, which is the best antibiotic for tooth infection according to current dental guidelines, how each one works, and what you can do to protect your oral health going forward.
Whether you’re dealing with a dental abscess right now or want to be prepared, this article will give you clear, trustworthy answers based on evidence and expert recommendations.
Do you actually need an antibiotic for a tooth infection?

This is the most important question, and the most misunderstood. The truth is, antibiotics are not the first line of treatment for most tooth infections.
The American Dental Association (ADA) and the World Health Organization (WHO) both caution against overprescribing antibiotics because of growing concerns about antibiotic resistance.
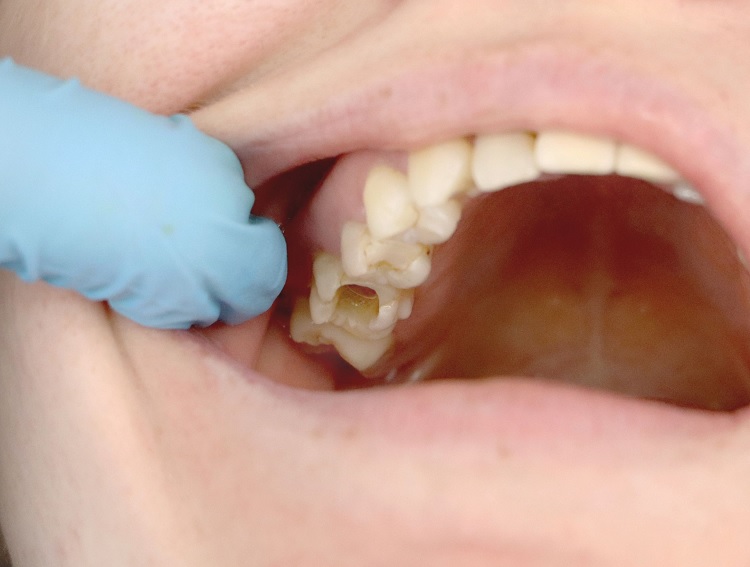
A tooth infection is caused by bacteria invading the pulp (the nerve and blood vessel tissue inside the tooth). This can result from untreated cavities, a cracked tooth, failed root canal therapy, or advanced gum disease. The infection may stay localized inside the tooth or spread to surrounding bone and soft tissue.
When dentists prescribe antibiotics for tooth infections
Antibiotics are typically reserved for specific situations, including:
- The infection has spread beyond the tooth to nearby tissues, lymph nodes, jaw, or neck
- The patient has a weakened immune system (diabetes, cancer, HIV, lupus, or recent organ transplant)
- There is significant facial swelling, fever above 101°F (38.5°C), or difficulty swallowing
- The patient is at high risk for bacterial endocarditis (heart valve conditions)
- Initial dental procedures alone, like drainage or root canal, have not controlled the infection
In many cases, procedures like dental drainage, a root canal, or tooth extraction can eliminate the infection without antibiotics at all.
Antibiotics treat bacteria, but they cannot drain a pocket of pus or remove infected tissue, that’s a job for dental instruments.
Best antibiotics for tooth infection: a complete guide

When an antibiotic is truly needed, choosing the right one depends on the type of bacteria present, the patient’s medical history, and any known allergies.
Here is a breakdown of the antibiotics most commonly prescribed for dental infections, based on ADA guidelines and current clinical evidence.
Amoxicillin: the first-line choice
Amoxicillin is considered the best antibiotic for tooth infection in most patients without penicillin allergies. It belongs to the penicillin family and works by disrupting the cell wall of bacteria, effectively stopping their ability to multiply and survive.
- Typical dose: 500 mg three times daily for 5–7 days
- Effective against: a wide range of oral bacteria including Streptococcus and anaerobic species
- Important: Not effective against viral infections, only bacterial ones
- Avoid if: you have a penicillin or amoxicillin allergy
When bacteria show resistance to standard amoxicillin, dentists may prescribe amoxicillin with clavulanic acid (sold as Augmentin). The clavulanic acid prevents bacteria from breaking down the antibiotic.
Note: this combination may reduce the effectiveness of oral contraceptives.
Clindamycin: best alternative for penicillin-allergic patients
For patients who are allergic to penicillin, clindamycin is often the preferred alternative.
- Typical dose: 150–300 mg every 6 hours
- Effective against: anaerobic bacteria commonly found in dental abscesses
- Caution: do not combine with azithromycin, they block each other’s effects
- Monitor for: antibiotic-associated colitis (Clostridioides difficile infection)
A 2015 study published in peer-reviewed dental literature highlighted clindamycin’s effectiveness against dental bacteria and noted relatively low bacterial resistance compared to other alternatives.
Azithromycin: short-course option
Azithromycin is sometimes prescribed for patients who cannot tolerate penicillin or clindamycin.
- Contraindicated in: patients with liver disease
- Do not combine with: clindamycin (opposing mechanisms cancel out)
Azithromycin’s main advantage is a shorter treatment course (typically 3–5 days). However, it has higher rates of bacterial resistance than amoxicillin.
Metronidazole: often combined, not first-line alone

Metronidazole is particularly effective against anaerobic bacteria, the oxygen-hating microbes that thrive deep inside dental abscesses.
- Avoid with: alcohol (severe nausea reaction), anticoagulants, seizure medications
- Caution in patients with: liver disease, nervous system disorders, or blood cell disorders
Metronidazole is frequently used in combination with amoxicillin for more severe infections rather than as a standalone first-line treatment.
Cephalexin: another penicillin-allergy alternative
Cephalexin is a cephalosporin antibiotic that works by inhibiting bacterial cell wall synthesis.
- It is useful when amoxicillin cannot be used, though it is structurally similar to penicillin and may cause cross-reactions in some penicillin-allergic patients.
- Avoid in: patients with kidney failure, liver disease, or during pregnancy
Erythromycin: older option, limited use today
Erythromycin has largely been replaced by newer antibiotics due to higher bacterial resistance.
- It is still occasionally used for treatment of cavities-related bacterial infections and some dental abscesses, primarily when other options are not suitable.
- Avoid with: terfenadine, astemizole, or cisapride (dangerous drug interactions)
Side effects of antibiotics: what to watch for

All antibiotics carry a risk of side effects. Most are mild and resolve after treatment ends, but some require immediate medical attention. According to the U.S. National Library of Medicine, common side effects include:
- Nausea, vomiting, or diarrhea, especially on an empty stomach
- Yeast infections (oral or vaginal candidiasis), antibiotics disrupt your natural bacterial balance
- Headache or mild dizziness
- Skin rash or hives
Seek emergency care immediately if you experience: difficulty breathing, severe facial or throat swelling, or rapid heart rate, these may indicate a serious allergic reaction (anaphylaxis).
⚠️ Important: Antibiotics fight bacteria, but they do NOT relieve tooth pain. Ask your dentist about appropriate pain management alongside your antibiotic treatment.
Preventing tooth infections before they start

The best antibiotic for tooth infection is the one you never need. According to the WHO Global Oral Health Report (2022), approximately 3.5 billion people worldwide are affected by oral diseases, the vast majority of which are preventable. Over 2 billion adults have untreated cavities in permanent teeth.
Here are evidence-based steps to protect your oral health:
- Brush twice daily with fluoride toothpaste for at least 2 minutes each session
- Floss or use interdental brushes daily to remove bacterial plaque between teeth
- Limit sugar and acidic foods, especially between meals
- Use xylitol (birch sugar) as a substitute — studies show it inhibits the bacteria that cause cavities
- Visit your dentist at least twice a year for professional cleanings and X-rays
- Treat dry mouth promptly — reduced saliva increases infection risk significantly
- Replace your toothbrush every 3 months or after illness
What products can I use to help improve my oral hygiene?
These products can support your oral health before, during, and after dental infection treatment. Always consult your dentist before use.
These suggestions are for informational purposes only and do not constitute a medical prescription.
A clinically tested antibacterial rinse that reduces oral bacteria without irritating sensitive gums or tissues.
It is ideal for patients recovering from a dental infection or abscess, as it helps reduce the bacterial load in the affected area without aggravating pain.
A professional-grade electric toothbrush featuring pressure-sensing technology and brushing modes.
Effective plaque removal is your primary defense against dental infections. It is clinically proven to remove 100% more plaque than manual brushing.
A comprehensive oral hygiene kit including interdental tools designed to clean between teeth and along the gumline.
Interdental cleaning removes bacteria from areas a toothbrush cannot reach, which is a critical step in preventing the abscesses and gum infections that require antibiotic treatment.
Frequently Asked Questions
What is the best antibiotic for a tooth infection?
Can a tooth infection go away without antibiotics?
How long does it take for antibiotics to work on a tooth infection?
Can I take over-the-counter antibiotics for a tooth infection?
Do antibiotics stop tooth pain?
Voice and Search (Q&A)
Do I need antibiotics for every toothache?
No. Antibiotics are not the first line of treatment. Most tooth infections require dental procedures, such as drainage, root canals, or extractions, to remove the source of the infection. Antibiotics are only used if the infection has spread or if you are at high risk.
When should I seek emergency care?
Seek immediate medical attention if you experience severe facial or throat swelling, difficulty breathing, high fever, or a rapid heart rate, as these may indicate a life-threatening allergic reaction or a rapidly spreading, dangerous infection.
How to manage dental pain while waiting for a dentist appointment?
While waiting for your appointment, you can manage pain with over-the-counter anti-inflammatory medications like ibuprofen, provided they are safe for you. Avoid hot or cold triggers, and keep your head elevated.
Share
References
1. Burgess, L. (2025, February 13). Are there natural ways to remove cavities at home? https://www.medicalnewstoday.com/articles/321259
2. Chao, S. (2025, January 23) What are the best antibiotics for a tooth infection?. https://www.drugs.com/medical-answers/best-antibiotics-tooth-infection-3555997/
3. Contaldo, M., D’Ambrosio, F., Ferraro, G. A., Di Stasio, D., Di Palo, M. P., Serpico, R., & Simeone, M. (2023). Antibiotics in Dentistry: A Narrative Review of the Evidence beyond the Myth. International Journal of Environmental Research and Public Health, 20(11), 6025. https://doi.org/10.3390/ijerph20116025
4. Dorwart, L. (2026, March 4) How Quickly Do Antibiotics Work for Tooth Pain From Infection?. https://www.verywellhealth.com/antibiotics-for-tooth-infection-5220697
5. MedlinePlus (2024, July 20) Amoxicilin and Clavulanic Acid. https://medlineplus.gov/druginfo/meds/a685024.html
-
Dr. Yeidy Carolina Mesa [Author]
DDS Yeidy Carolina Mesa Passionate Dentist | Advocate for Accessible Oral Health Education Graduating from Universidad CES in 2022, I am a dedicated general dentist with a lifelong passion for helping others and making a meaningful impact in the world. My journey into dentistry began at the age of 7, inspired by my own experience with braces and overcoming a fear of the dentist. This personal journey shaped my mission to help patients conquer their own dental anxieties and embrace a healthier,...
View all posts
-
Nayibe Cubillos M. [Medical Reviewer]
Pharmaceutical Chemestry |Pharmaceutical Process Management | Pharmaceutical Care | Pharmaceutical Services Audit | Pharmaceutical Services Process Consulting | Content Project Manager | SEO Knowledge | Content Writer | Leadership | Scrum Master
View all posts
A healthcare writer with a solid background in pharmaceutical chemistry and a thorough understanding of Colombian regulatory processes and comprehensive sector management, she has significant experience coordinating and leading multidisciplina...Recent Posts